- Latest Update: 3/8/2022 – Added new video from Gez Medinger at Healthcare Conference
- Original post date: 10/13/2020 (Change Log at bottom of the article)
Update 11/4/2021 – My radio interview on OPB (NPR) along with fellow long-hauler, Amy Watson from 10/28/2021.
Update 10/28/2021 – At this point, I would call myself about 98% recovered. My days are mostly normal with the occasional flare-up that I can generally work through at this point. I am still careful about exercise and diet and I still take supplements including Vitamin D, Allergy meds, Pepcid AC (Famotidine), and a multivitamin, but that’s about it. My focus has switched back to game development as I try to leave this awful yet educational and life-affirming experience behind me. I think the experts were right when they estimated that most people suffering severe Long Covid would take between 12 to 18 months to fully recover. While the largest changes in my recovery happened around month 5, the rest has improved very, very slowly over time. I think my lingering tinnitus and temperature dysregulation will eventually fade out too, but they just take longer.
I’ve also been practicing neuroplasticity exercises whenever I feel like I might be experiencing the start of relapse. This is a bit tough to describe, but I will do my best. If you are a long-time long hauler, your brain has developed a subconscious habit of triggering a response to even mild changes in your body. It’s a form of PTSD. When I feel these feelings coming on, I quickly take about 10 slow deep breaths with even slower exhales. Sometimes I follow that up with a walk. This provides stimuli that tell the subconscious that “things are ok” and no immune response is needed. While this doesn’t seem to work 100% of the time, it DOES seem to work some of the time. Try it out to see if it works for you. If you are still in the early phases of Long Covid, I am doubtful this will be effective at shutting down relapses but it’s definitely good practice for calming your subconscious.
While this post is a departure from game-related content, I thought this was important to post since I believe this could help some people going through what I’ve experienced since the beginning of March 2020. This Covid-19 Long-Hauler Recovery post is a work in progress that I will continue to update with new information as it emerges. I created this document to share some of the things I’ve learned during my 14-month struggle (and counting) with Chronic Long Covid-19.
If you had Covid-19 and have been suffering from symptoms for a month or longer, check out the new Long Hauler program offered by Dr. Yogendra and IncellDX. Note: We have no affiliation with the program and do not benefit in any way. I received my results back in November, which shows inflammation markers 45 times higher than normal. My results from April showed a reduction in most of my inflammation markers but I still had elevated VEGF and CCL5 (RANTES). More details on this are explained below under the Resources For Long Haulers section.
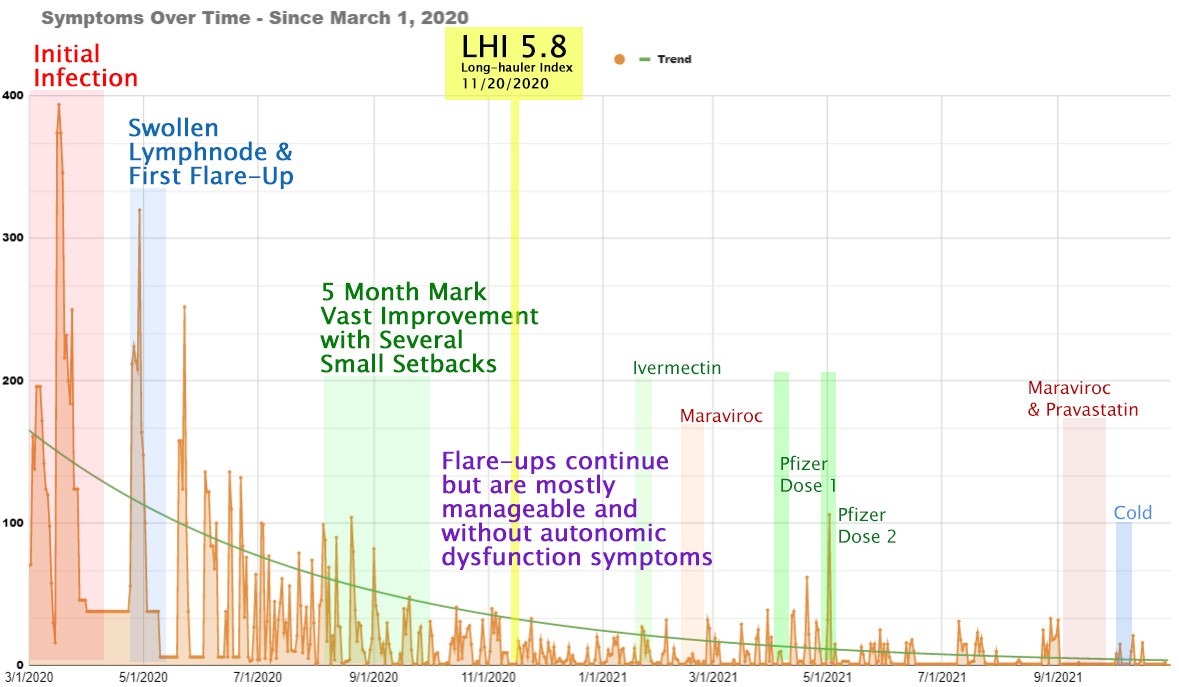
The best way to describe my Covid experience to other traumas I’ve endured would be that of a severe concussion or head trauma. I’ve experienced several head injuries and concussions in my life, but never one as significant as Covid. My initial Covid-19 experience was a combination of arrhythmia, horizontal intolerance, autonomic dysfunction, panic attacks, anxiety, shortness of breath, loss of smell and taste, myalgia, horrible pressure inside my head that felt like I had been hanging upside-down for hours1, burning sensations in my head, chest and arms, confusion, and what felt like poison running through my veins. Someone in an interview put it perfectly saying “I feel like I’ve been placed in someone else’s body.” My Long Covid experience has been a lot of the same symptoms listed above that come in waves and then fade and then come back over and over again (See my symptom tracker below).
Table of Contents
Symptom Tracker
Symptom Tracking Sheet – Track your daily progress with this Excel document or this Google document. They are essentially the same document. Feel free to use and share whichever you like. Each will create a chart that displays your overall health trends like the one I created below for myself.
 |  |
| Google Sheets version of Health Tracker | MS Excel version of Health Tracker |
What is Chronic Covid-19?
Also known as Long Covid, Long-term Covid, and Covid long haulers, Chronic Covid is a condition where the patient’s body does not recover from the disease within the established 10-14 day infection period. People with Long Covid suffer for weeks or months or possibly longer and some have permanent damage to their lungs and other organs. This post is focused on the non-specific multi-system impact of the disease.
Here is how it’s described by the CDC. While it’s unclear what percentage of people are affected by Chronic Covid, the most recent estimates I’ve heard are:
- 33% of people will experience symptoms lasting over 2 weeks after the initial infection.
- 10% of people will experience symptoms lasting 2 months or longer after the initial infection.
Not all Long Haulers are the same since some were hospitalized and experienced organ damage due to the massive immune response to the virus, while others experienced mild to moderate disease treated with OTC medications at home. Since I belong to the mild to moderate camp, this article is focused on long haulers who did not experience any known organ damage.
Here is a great, quick primer on Chronic Covid by a fellow long hauler.
This type of sequelae is not uncommon with acute viral infections as similar studies reveal with people infected with SARS and MERS. Even seasonal flu and colds can cause this aftershock-like effect on the body. While it’s currently unknown what causes this condition, there are a few popular theories.
I now believe that all three of these theories play a part in various phases of Chronic Covid-19.
Overactive immune system – This theory makes a lot of sense to me, both based upon my own slow recovery and the fact that many Long Covid patients have recovered after taking Methylprednisolone steroids. More on this is under the Prescription Medications section below. This is also consistent with Mast Cell Activation Syndrome (MCAS) which is described in detail below.
Immune System is responding to viral debris – This theory assumes that the dead RNA virus spike proteins are lingering in the body and setting off an immune response as the body’s organs cycle through it all. I personally believe that everyone who has recovered from Covid has some viral debris or even some viral persistence, however, it just doesn’t bother people who don’t have MCAS. This is just my own theory though, so “grain of salt.”
The virus is still active – This is the theory that scares the heck out of Long Haulers. Many believe the virus is still active based upon the number of new symptoms that spring up each time they experience a flare-up. The latest findings by Dr. Patterson suggest that there is likely viral debris that is NOT viable for replication but can set off the immune response when detected.
Viral Debris Mobility [Update 5/13/2021] – The new working theory by Dr. Patterson believes that activities like exercise can set this viral debris in motion and result in a flare-up. This aligns with my own experience with post-exertional malaise. There is always a 24-72 hour delay between exercise and a flare-up for me. I think that inflammatory foods can also provide some mobility to this viral debris since inflammation can unsettle things in your system.
This theory correlates Chronic Covid-19 with NAD+ depletion. This is explained in great detail in this article by Nikita Alexandrov, BChem, MBA on Medium. If you are unable to open the full article, I suggest trying in incognito mode. While many long haulers have shown benefit from taking Niacin, I am not one of those. I have really only suffered from the post-exertional malaise form of ME/CFS and have not experienced the crushing fatigue that others describe. I think Niacin may help people with fatigue more than those with malaise, but I’m only guessing based upon my own experience.
The theory mentioned above was recently discussed on RUN-DMC’s channel below. If you haven’t already subscribed, I highly recommend you subscribe to his channel. If you are wondering, his channel is named RUN-DMC since he is a runner and a DeLorean DMC-12 enthusiast. There is a Part 2 to the video below that should appear after the video below ends.
Why Are Some People Develop Chronic Covid-19 and Others Don’t?
A recent self-reported study revealed that there are several pre-existing conditions that could lead to chronic Covid-19.
These pre-existing conditions include:
- Atopic Asthma (157% increased risk)
- Rheumatoid Arthritis (1500% increased risk)
- Post-Viral Syndrome (6000% increased risk)
Adding one more possible factor from other sources:
- Poor Gut Health – See Gut Health section below
What Does Chronic Covid-19 Feel Like?
I can only speak for myself even though my symptoms align with thousands and thousands of others, but I have two sets of symptoms. One set is a constant, no matter how I am feeling and the others only occur during weekly flare-ups. I didn’t list every one of my symptoms below, just ones that really stand out to me that aren’t directly related to greater symptoms, like dizziness and vertigo as part of autonomic dysfunction. I experienced anosmia during my first few weeks of the virus, but thankfully my smell and taste came back after that. I’ve also experienced diarrhea at times, but those times haven’t all aligned with flare-ups.
Vaccine Results [New 5/13/2021]
I received my first dose of the Pfizer vaccine on April 10 and about 24 hours later I was hit with the most severe fatigue I’ve ever experienced. I woke up around 2am and was extremely dehydrated. Even though my water bottle was less than 5 feet from my bed, I didn’t have the energy to get up and retrieve it. The severe fatigue subsided by the following afternoon, but fatigue came and went over the next 2 weeks and I started experiencing more flare-ups than usual. I felt as though my long hauler recovery took a two-month step back into the symptoms until after I received my second dose.
My second dose of Pfizer came on May 1 and within about 12 hours I felt very sick, but not with any of the scary symptoms I experienced with Long Covid. I ran a fever between 100 and 101.5 degrees Fahrenheit for about 36 hours straight. I also experienced a severe headache that seemed to move around my skull as well as body aches. I decided not to take any medications as I really wanted the vaccine and my immune system to do their jobs unimpeded.
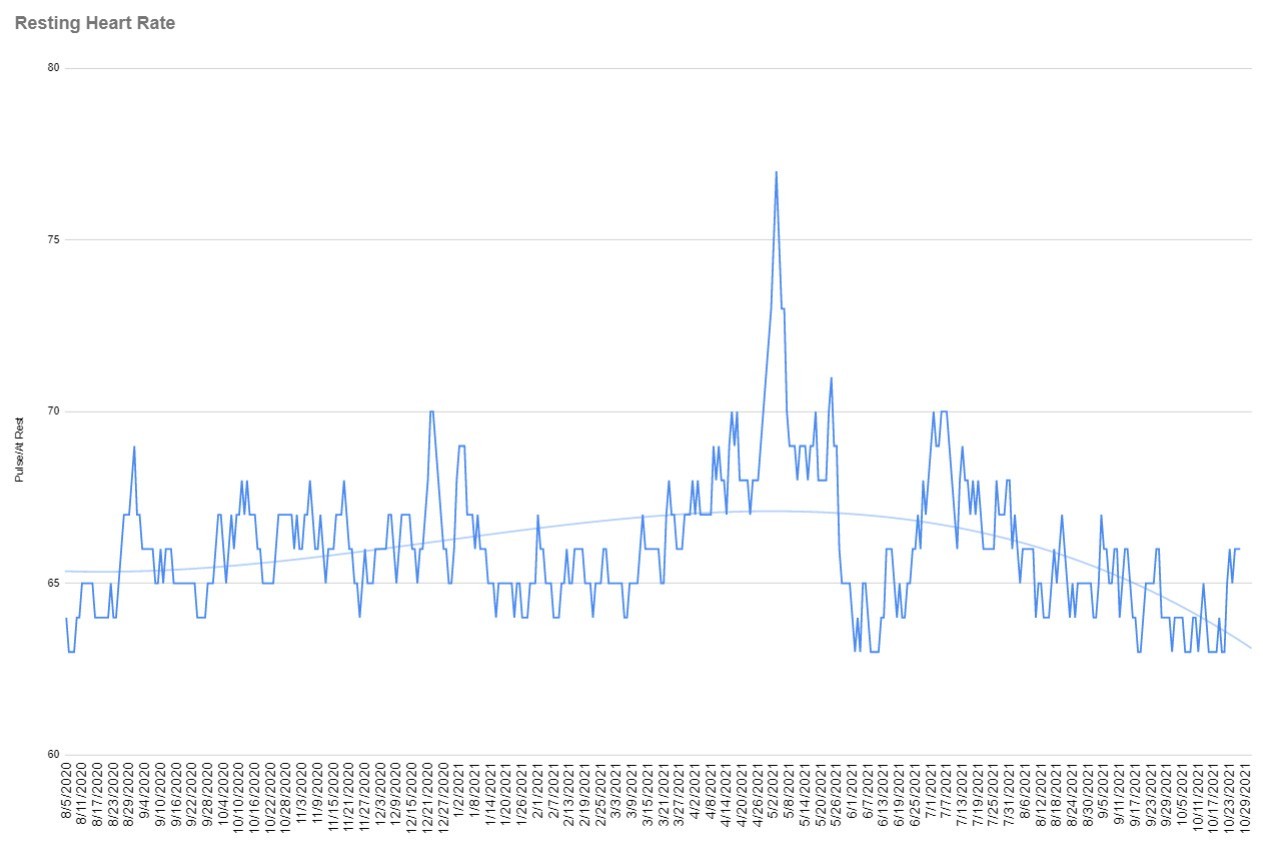
The first thing I noticed after taking the second dose, aside from the symptoms, was that my resting heart rate shot up significantly. Usually, when it goes up even one or two beats per minute, I wind up having a flare-up within a day or two. But not this time! Even though it jumped to by far the highest number I’ve ever seen since I started paying attention, I didn’t experience a flare-up. The other thing I noticed is that my sleep has improved significantly. I’m not sure if that has anything to do with taking the vaccine or just time.
Gut Health & Secondary Infections
Some recent studies have linked poor gut biome with severe cases of Covid and Chronic Covid.
- American Society for Microbiology article
- The BMJ article
- NIH article about the Gut’s impact on Cardiovascular Health
- SpringerLink’s article about the role of probiotics to combat Covid-19
I strongly recommend taking a good probiotic and cutting out sugar no matter what your current condition. Getting your gut back into shape will likely take quite a bit of time and more than just diet change and cutting sugar. Naturopathic doctors could be a good place to start, but make sure you do your homework before signing up with one. They tend to be expensive, some are shady with lots of upsells, and insurance coverage is spotty.
When talking to your doctor or specialists, make sure they are aware of potential secondary infections that can occur after an acute illness. When the immune system is hammered, bad bacteria or other things that usually maintain equilibrium can get thrown out of whack and result in an infection or overgrowth leading to more unpleasant symptoms.
I discovered that I have gastritis and inflammation of the stomach and intestines after having an endoscopy. They originally suspected a bacteria overgrowth in my small intestine (SIBO) but did not find any concerning bacteria, like h. pylori, just inflammation. My treatment includes probiotics and a low FODMAP diet for the next several weeks at least. I am certain I had poor gut health prior to my infection, which could contribute to the reason why I’m a long hauler.
I noticed that most of my GI symptoms seemed to go away after taking my prescribed round of Ivermectin and Maraviroc. At this point, I’m convinced that one or both of these drugs fixed my gut issues as I have not experienced them since and that was 7 months ago now (10/28/2021).
My Constant Symptoms
Due to the inflammatory nature of the virus, it seems to exacerbate some symptoms you may already have had but never noticed. If you have a little allergy problem; you now have a big allergy problem. If you have minor aches and pains; you now have severe and often terrifying aches and pains. And so on.
Tinnitus – Absolutely unrelenting tinnitus since March in both ears. This intensifies right before and during a flare. I have learned to treat it as an alarm system. When it starts getting loud, which is usually accompanied by pressure changes in my ear similar to changing altitude, I know that I need to rest until it passes or risk a lengthy flare.
Temperature Dysfunction – My hands often get ice cold while my core temperature feels warm to me. When I take my temperature with a thermometer wand, it varies greatly across different sections of my head and body. My hands are often too low of a temperature to register while my core temperature appears normal.
Blurry Vision – The near-sight of my left eye has been blurrier than my right eye since I got sick at the beginning of March and has not improved. I went to an ophthalmologist and he told me that it must be neurological since there was nothing physically wrong with either of my eyes.
Horizontal Intolerance (Lasted roughly 3 months) – This was my most confounding early symptom that we assumed was PTSD until I spoke to Dysautonomia experts. Every time I laid down horizontally, my body would go into a panic attack with tachycardia and heart palpitations. The symptoms would quickly subside after I sat upright. It took about three months of sleeping upright before I eventually got past it.
My Flare-up Symptoms
Mast Cell Activation Syndrom (MCAS)
I believe my flare-ups are a form of Mast Cell Activation Syndrome. Covid-19 seems to mimic many different illnesses like POTS, Dysautonomia, and Mast Cell Activation for certain durations of time. I found it very interesting that Mast Cell Activation can result in POTS and Dysautonomia symptoms as well. This leads me to believe that what I have been experiencing is the over activation of mast cells to varying degrees throughout the course of this dreadfully drawn out illness due to system-wide hyper-inflammation. It seems that my pre-Covid system was at an inflammation level of around 1 out of 10; shot up to 10 our of 10 during Covid and has been slowing coming back down to normal levels, but at different rates throughout my body. So it doesn’t take much to set off a flare-up when I’m still inflamed, albeit, some minor allergy I might not have ever known I had because it had never set off any noticeable reaction… until now that I’m starting from hyper-inflamed state.
Fatigue or Malaise – I’ve always referred to this more as extreme malaise because I feel incredibly sick when the fatigue hits. I feel more flu-like sick than I feel tired, but I’ve been told that this is what “fatigue” is generally referring to by other chronic Covid-19 sufferers. Weakness is something else that occurs during these flare-ups that I put into the same category as fatigue. I have not experienced the crushing fatigue (extreme tiredness) that many sufferers experience.
Shortness of Breath – This symptom would crop up every time I had a flare-up. It was also one of my first Covid-19 symptoms recognized back in March, but like so many at the time, I assumed that Covid-19 shortness of breath was due to pneumonia and not the vascular issues that actually cause it. Famotidine was the gamechanger for me for my shortness of breath. Just one 20mg pill got me over it within 24 hours. I haven’t had an issue with it in months since then.
Blood Pressure Changes – Still related to autonomic dysfunction, my blood pressure will drop when I stand and walk around which results in vertigo and dizziness. It takes 5-10 minutes sometimes before my blood pressure starts functioning properly while standing.
Brain Fog – I would describe the brain fog I experience more like brain pressure at times, especially earlier in my illness. It is extremely anxiety-inducing when the pressure feels really intense, almost like your head is going to explode or like you’ve been hanging upside-down for hours. Thoughts tend to race and it’s nearly impossible to complete a task or even focus on a single thought for more than a few seconds. While this has greatly improved over time, I still have bouts with it during flare-ups now. For some reason, my brain fog generally comes immediately after my fatigue and seldom at the same time. Fluvoxamine has recently been discussed as a potential prescription to help alleviate brain fog.
Burning & Tingling Sensations – I get these really uncomfortable burning sensations in my head, chest, and forearms during most flare-ups, although these have faded significantly over the past couple of months. I believe it is all related to inflammation as my lungs will occasionally wheeze when this happens. Dr. Bruce Patterson and Dr. Yogendra believe this is due to an increase in Vascular endothelial growth factor (VEGF). VEGF is a signaling protein that promotes the growth of new blood vessels. Gross!
Elevated VEGF causes peripheral neuropathy, burning sensations, and brain fog!
Anxiety – I’ve never experienced the physical type of anxiety before contracting this disease. I’ve been through highly stressful events in my life, but never felt anything more than slight butterflies or nervousness. Never anything remotely close to the anxiety I started feeling after my infection. Later I learned that this is another physical manifestation of Mast Cell Activation.
The body will counter-act histamine by producing Epinephrine (adrenaline) which helps to de-activate histamine. Sometimes high levels of adrenaline can result in unwanted anxiety and panic attacks.
http://sepa.duq.edu/regmed/immune/histamine.html
Psychiatric: Common psychiatric symptoms include anxiety (sometimes even to the point of panic), depression, mood lability, anger, attention deficit, and a wide variety of aspects of cognitive dysfunction, most commonly issues with memory, word-finding and concentration. “Disassociation” or “depersonalization” is occasionally seen. Frankly psychotic behaviors (e.g., auditory or visual hallucinations) are fairly uncommon.
Clinical Manifestations Of Mast Cell Activation Syndrome By Organ Systems
If mast cells activate in your GI tract, you can get nausea, stomach pains, diarrhea or vomiting. If they activate in your brain, you can get anxiety, depression, irritability, and fatigue. If they activate in your skin, you can get rashes, hives, and itching.
drtaniadempsey.com
Myalgia – For the first five months of my flare-ups, I would get extremely painful myalgia in my forearms and occasionally in my elbows and hands as well. It felt like a deep ache, like deep in the bones. Ibuprofen seemed to help with this to some degree when it occurred. Thankfully, I haven’t experienced much of this for the past few months. “Elevated IL-6 causes muscle & joint pain.” – Dr. Patterson, IncellDX
Gastrointestinal Issues – I experience on and off bloating, discomfort, and unforgiveable gas. I’ve noticed a marked improvement after taking Ivermectin and Maraviroc, but I’m cautious to say whether or not they were the cause of this positive change.
Blurrier Vision – In addition to my already left eye blurriness, both of my eyes get significantly blurrier during a flare-up.
Hoarse Voice – Due to what I assume is inflammation, my voice will get noticeably weaker and hoarse.
The 5 Month Mark
As you can see from my symptom tracker above, the largest change for the better in severity came in month 5 of the illness. I’ve heard this from many other long haulers as well. There are things you can do to help your body heal, like a low inflammatory diet, no alcohol, and paced exercise, but time is a thing we can’t control. Like every bruise, break, or sprain, your body requires time to heal itself.
5 months was the mark where I no longer felt like things were out of control and I felt markedly getting better. While I was still having bouts with brain fog during flares, my day to day thoughts became what felt like my own again. While this isn’t true for every long hauler, especially those with tissue damage, it seems to be the case for a lucky lot of us. I know there are many people out there that may be reading this that are past the 5-month mark without improvement and I feel for them. It likely just means things will take a little bit longer for some people. The good news is that there are a LOT of resources looking into this, so help is on the way.
Long sufferers of ME/CFS could also be getting the help they’ve needed for years as a result. They have every reason in the world to be furious that it’s taken a global pandemic to be taken seriously and get them the help they’ve deserved for so long.
Alcohol
I have avoided all alcohol since getting sick in March since the few times I drank wine or beer I paid a heavy relapse price the following day. I recently heard about vodka and whiskey having the opposite effect for some long-haulers in the Covid Long Hauler’s reddit group. I gave whiskey a try and was shocked that I actually felt good the entire time I was drinking. I wound up drinking near half a bottle on NYE and did not experience either a hangover or flare-up for two days, so I thought I was out of the woods. However, I wound experiencing my most lengthy flare-up in months for the next 6 days. While I’m not certain it was the whiskey that caused it, it is the most obvious thing. So if you decide to give it a try, please proceed with heavy caution and know that your flare-up might not hit you right away.
Resources For Covid-19 Long Haulers
New Chronic Covid-19 Center Program – Just launched by Dr. Bruce Patterson and Dr. Ram Yogendra (Dr.Yo). Please watch the video below for details and visit their new site to sign up. Word of advice: If you wish to participate in this program, please make sure you have all the required materials and verify with your lab before heading there and waiting for 2 hours just for them to tell you “no.”
I just received my results from bloodwork I sent back in November. They got very backed up for a period since they were finding new external labs to help process everyone’s results. The use a Long Hauler Index scale from 0 to 20. 0 means you are fully recovered while 20 is the most severe as Dr. Yo explains in the above video. I registered as a 5.8 on this scale at the 8-month mark showing 45 times the normal rate of inflammation. Dr. Bruce Patterson has prescribed me a week’s worth of Maraviroc and Ivermectin to start. They may follow up with a tapered round of Prednisone if my inflammation markers are still high.
My Experience With The New Covid Long Hauler Program
My bloodwork was received by IncellDX on November 17, 2020. It was nearly two months before I received my results back, but I had submitted before they were fully set up and had the lab resources that they now have today. You should not expect this long of a delay going forward from what I’ve been told.
| Average (pg/ml) | TNF-α | IL-4 | IL-13 | IL-2 | GM-CSF | sCD40L | CCL5 (RANTES) | CCL3 (MIP-1α) | IL-6 | IL-10 | IFN-γ | VEGF | IL-8 | CCL4 (MIP-1β) |
| Normal Values | 9.09 | 4.18 | 3.94 | 6.17 | 51.27 | 7192.39 | 10781.84 | 22.82 | 2.21 | 0.67 | 1.94 | 9.32 | 16.87 | 76.84 |
| My Values | <4.84 | 14.39 | <3.07 | 14.22 | <5.51 | 5389.3 | 14172.25 | 99.62 | 17.93 | 11.02 | 77.00 | 42.10 | <15.74 | 15.71 |
I was provided the chart above and told that my long hauler index is 5.8 out of 20. I have been prescribed a two-dose course of Ivermectin and a week’s worth of Maraviroc. After treatment, I’ve been advised to send in my bloodwork again for analysis. If I am still having symptoms and showing inflammatory markers, they will likely prescribe me a round of Prednisone. Ivermectin, Maraviroc, and Prednisone are covered in more detail in the prescription medication section below.
Pulmonary Wellness Covid Bootcamp – This is a FREE program that guides you through a daily gentle exercise to retrain your body. These include extremely useful breathing exercises for all occasions and body movements that help open up your lungs and heal your nervous system. There are also great webinars and lectures with top medical professionals and scientists. You can read a lot more about Dr. Noah Greenspan and his foundation in this article I co-authored with him back in August.

Survivor Corps – They provide a litany of materials, webinars, reports, and Post-Covid Post-Covid Care Centers.

My Results From The Medications Prescribed From IncellDX’s Long Hauler Program [Updated 5/13/21]
- Ivermectin (“Stromectol”) – After completing a two-dose course of 12mg Ivermectin 4 days apart, I did not notice any improvement of my daily symptoms or any less severity or duration of my flare-up symptoms. However, my gut health seemed to improve by a significant amount. It’s unclear if Ivermectin or Maraviroc or just time made the difference, but I would credit these drugs with being the most likely cause. The benefits of Ivermectin are described in the Prescription Medication section below but include an antiviral effect as well as immunomodulation along with the anti-parasitic properties that the drug is most well-known for.
- Maraviroc (“Selzentry”) – This HIV drug was prescribed to me for at 300mg twice daily for one week. This is an antiviral drug with immunomodulation. This drug is extremely expensive without a pharmacy prescription – $360 just a week’s worth! Dr. Patterson and Dr. Yogendra have mentioned they can refer patients to affordable pharmacy prescriptions (https://www.viivconnect.com/) which will save them a lot of money on this drug. I started experiencing a flare-up during day 3 of the treatment, but it was not significant enough to really disrupt my day. As mentioned under the Ivermectin section, my GI issues vastly improved after the course of both drugs. It was about a week or two after the courses that I noticed this improvement, so if you are prescribed these don’t assume they aren’t working because you aren’t noticing instant results.
Keys To Recovery [Updated]
Sleep, Sleep, and More Quality Sleep [Updated 5/13/21]- This is probably the most important thing you can do to improve your symptoms and overall recovery time. It’s not easy since autonomic dysfunction causes sleep disturbances and can exacerbate pre-existing conditions like sleep apnea. If you are having difficulty getting quality sleep, I highly recommend talking to a sleep specialist who can give you an overnight monitor to identify the problem. I started using a Fitbit with sleep monitoring as well to help track my nightly sleep patterns. While they aren’t as good as a prescribed sleep monitor, they will give you a decent picture of your sleep patterns. It can be a bit of a double-edged sword if you feel like you slept well, but the device says otherwise. It can psychologically convince you that a good night’s sleep wasn’t so good and make you feel tired as a result. I have noticed a vast improvement in sleep since taking the vaccine. This improvement didn’t start until about a week after my second dose of Pfizer. I am staying asleep through most of the night now after over a year of waking up dozens of times throughout the night.
Stay Hydrated with Electrolytes – Dehydration drives blood pressure swings and adrenaline excess. Water alone won’t help, you need electrolytes to replenish your depleted system. Too much water without electrolytes can actually make things worse. Gatorade, Electrolyte water, coconut juice are all good options.
Reduce Stress – This can be extremely difficult to do during a global pandemic during some of the most divisive times in our history. However, you can control some aspects of your life that bring on stress and anxiety.
- Limit your time watching the news
- Limit your time engaging in support groups where people are generally posting on their worst days.
- Limit talking to people who stress you out for one reason or another.
- Get outside for at least ten minutes every day to keep yourself grounded in nature.
- Not every ache and pain you feel is related to Covid. It’s normal to feel random aches and pains throughout a normal healthy day.
- Tell yourself that like all things, this will pass in time.
Low Inflammatory Diet – While your body is recovering from a highly inflammatory illness, it’s important to keep inflammation to a minimum as much as possible. One of the most important ways you can control this is by adopting a low inflammatory diet. Another thing you might consider is intermittent fasting, which I started immediately after falling ill. The reason I started intermittent fasting was I read that when you stop eating many hours before going to sleep, your body uses your time asleep to repair your cells rather than digesting food.
Find a Good Doctor – I’ve heard many, many stories of doctors dismissing patients symptoms as “just anxiety.” While I don’t blame them since everyone has some level of anxiety during a global pandemic, physicians need to recognize the difference between general anxiety and physical symptoms resulting from autonomic dysfunction. There is now a good deal of material available that supports Chronic Covid. If your physician is unwilling to accept these well-established reports then it’s time to find a new doctor.
Pacing – Listen to your body and don’t overdo it. If you have any thoughts that you may be on the cusp of another relapse, don’t push it because you almost certainly will send yourself over the edge. A nurse mentioned a technique that records your heart rate immediately upon waking up in the morning. If it’s higher than usual, it could mean that you are on the brink. Heart monitors, like Fitbits, show your average resting heart rate each day. If you have a device like this, you should take note and see if increases in your daily resting heart rate coincide with ME/CFS-like flare-ups.
Time – This is one that we can’t control, unfortunately, but just like any other injury to your body it requires time to heal. As Dr. Noah Greenspan puts it, “it’s like your home was flooded with seawater and although the water is gone, the damage is still there.” Consider other injuries your body has sustained like a broken arm. You put it in a cast and allow it to slowly heal. The more you try using it, the longer it’s going to take to heal.
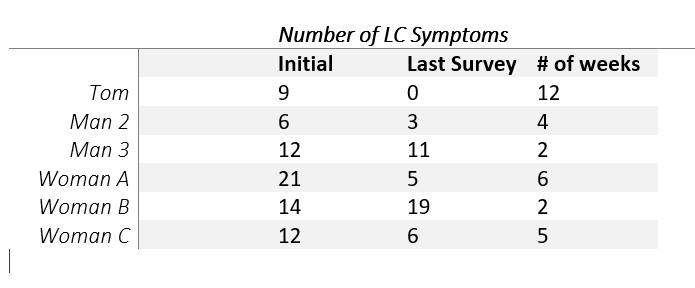
Intermittent and Extended Fasting – I started intermittent fasting in January of 2020, about two months before I got sick. I use the 16-8 method where I eat all meals within an 8-hour window allowing my body to digest the food and then heal for the remaining 16 hours of each day. Typically, I eat only between 8am and 4pm. Earlier this month, I learned about the role autophagy can play in hastening recovery and discovered this website created by a fellow long-hauler named Tom Bunker. He has now cured himself of long haul symptoms twice after becoming reinfected in October.
I decided to try a 72-hour water fast from December 18th to the 21st. Since I am already accustomed to intermittent fasting, the first 48 hours were not much of a problem for me, but by day 3 I had become quite hungry and had very low blood sugar levels. Other than the light-headedness, I was symptom-free during my fast and felt pretty good overall. I monitored my blood glucose levels and ketone levels throughout the fast. I didn’t reach heavy ketosis until the morning of the 3rd day. By the end, I lost 7 lbs and felt better than I have felt since before I got sick. I remained symptom-free for a couple of days before having a very mild flare-up. I have since followed up with two 48-hour fasts and again I was symptom-free during my fasts.
I credit a lot of my recovery to my multiple extended fasts.
He posts often to this Facebook Group that he manages and is showing promising results from other long haulers who are taking part.
What Supplements Have Helped You?
First of all, I need to be clear that none of this is medical advice and I am not advocating the use of any medication or supplement. I am NOT a doctor, I am just sharing my own anecdotal information that I believe helped me personally. The human body and immune system is incredibly complex and I don’t attempt to understand it. People can have vastly different reactions to supplements and medications, so read on at your own peril. All that said, if you are desperate for any relief like I was, and your doctors are providing helpful answers, you are looking for ANYTHING! Still, please, please, please always let your doctor know what you are taking or planning to take so that they can make sure it is safe specifically for YOU. There are all sorts of drug interactions that you may not be aware of that could be potentially deadly for even OTC drugs. Before getting into the details of each supplement, check out this recent video on the subject by RUN-DMC.
Famotidine (aka Pepcid AC) – This was the first game-changer for my shortness of breath symptoms. I started taking Famotidine at the end of June and my shortness of breath symptoms were gone by the next day. I only experienced mild symptoms of it since then during flare-ups. Not only does Famotidine help relieve excess stomach acid, but it is a histamine blocker (H2 blocker). Allergy antihistamines are H1 blockers. Since inflammation plays a massive part in Long Covid, any tools to calm that down is a plus. I generally have only taken a single 20mg pill per day, but have taken up to 2 20mg pills in a single day (40mg total). I was told by someone in a Facebook group that a Long Covid patient had an adverse reaction to Famotidine and had to be rushed to the hospital, so be careful and talk to your doctor.
Antihistamines – Regular allergy antihistamines are H1 blockers (histamine type 1). Since many of us suffer from some form of Mast Cell Activation Syndrome, taking antihistamines makes a lot of sense. Finding the right one for you will likely take some trial and error as our bodies respond quite differently. I have yet to settle on one that works for me but I’ve heard some good things about Cetirizine Hydrochloride. I just started taking it but have not noticed a difference yet.
Vitamin D3 – Vitamin D is not just a vitamin, it’s a hormone and a vital part of your immune system. It is estimated that 42% of people living in the United States are Vitamin D deficient. There numerous studies that link Vitamin D deficiency with poor Covid-19 outcomes and poor outcomes with other respiratory infections as well. Our main source of Vitamin D comes from the sun and it is not readily available in foods so supplements make a lot of sense here. How much Vitamin D3 should you take? I average about 4,000 IUs per day, which is the upper limit recommended, however, Dr. Mobeen prescribes 5,000 IUs for his patients. It’s best to take a blood test to determine your current level so that you take the appropriate amount. Age, body weight, and other individual factors apply to how much Vitamin D you need to take to maintain healthy levels. Toxicity of Vitamin D is possible, but recent studies have shown that it is rare to develop even after taking large doses for extended periods. My clinical results came back at an optimal 66.3 ng/mL of Vitamin D for me.
Quercetin – Quercetin benefits your vascular system, can reduce inflammation, and act as a zinc ionophore, which allows zinc to get into your cells and protect them from infection.
Selenium – Selenium is an immune booster and powerful antioxidant that may help reduce symptoms of asthma. Selenium can be found in Brazil Nuts as well as supplements.
Zinc – Zinc is key to immune health and used in abundance throughout your body. It is crucial to your Vagus Nerve function, so if you are having autonomic dysfunction issues as I experience, make sure you take a sufficient amount to help repair that.
Probiotics – Don’t skimp on these. Talk to your doctor, especially if you have a GI specialist available to recommend the right kind for you. Also, make sure you buy the right type as some can actually increase your histamine levels! If there was one thing I could change about my horrible recovery experience, it would be taking GOOD probiotics a lot earlier. I spent $150 on VSL3 which only lasted 20 days, but seemed to have a positive effect on my gut and overall health. My GI specialist recommended Align probiotics that are cheaper but still include the key good gut bacteria you look for in a probiotic. Another very specific probiotic recommended to me, that I’m still trying out, are L. reuteri Protectis children’s chewables.
Ubiquinol or CoQ10 – These are recommended by the Post Covid-19 Care video above as well and many other doctors to help to produce energy within the mitochondria “the energy powerhouse” of body cells. It is believed that acute viral infections can significantly deplete the mitochondria which leads to the ME/CFS-like symptoms that follow. Nancy Klimas, M.D. recommends taking either 200mg of Ubiquinol or 600mg of CoQ10 each morning. I had originally only taken 100mg of CoQ10 per day, but I am now increasing that to 600mg per day. I just replaced the CoQ10 with 200 mg of Ubiquinol this week. I haven’t noticed any meaningful difference so far.
Vitamin C – Good ole ascorbic acid is a great antioxidant for freeing your body of free radicals. This is also great for reducing the release of histamine in your system.
Black Cumin (Nigella Sativa) – This traditional medicine seed is known for its healing properties and its ability to inhibit proinflammatory cytokines that are related to Covid-19 and Chronic Covid-19 including TNFα, interleukin-1, interleukin-6, NF-kβ. I discovered this after watching a Dr. Been lecture regarding a new OTC treatment involving honey and Nigella Sativa seeds found here.
Omega-3 (High EPA/DHA) – Omega-3s are good anti-inflammatory supplements. They can also be found in many foods like fish, krill, and walnuts. Food, of course, is the best way of maximizing your absorption of nutrients. Dr. Paul Marik, the author of the MATH+ protocol for Covid-19 recommended this as well as a few other items found in this video.
Melatonin – I started taking 3mg melatonin for sleep months ago, but later found out that it has become a part of some Covid-19 protocols as well, including Math+ and the new I-MASK+ protocol.
NAC (N-Acetyl Cysteine) – Another powerful antioxidant, it is believed in some of the medical community that it can help shorten the length and severity of colds and flus. It is also a good fighter against free radicals, which can cause inflammation. It’s unclear how much of the pill form is actually absorbed into your body. I’ve taken anywhere from 3 to 6 of the 600mg pills a day for the last couple of months. While I have been improving, I don’t know if any of that improvement is due to NAC, time or some combination of a lot of things.
Cinnamon – Recommended by my friend and fellow long-hauler, Matt Clark. Matt found that cinnamon is a natural anti-viral. He cured himself and several other long-haulers by taking cinnamon with 3,000mg of NAC per day for a few weeks. Check out this article about cinnamon by the NIH. I continued having flare-ups after months of the combo because I believe my symptoms are primarily gut-related and likely due to a secondary infection like SIBO (small intestinal bacteria overgrowth).
Vitamin B1 (Thiamine) – This is another anti-inflammatory Vitamin that is widely available. I take about 3 100mg pills per day after seeing it recommended for long haulers on Dr. Been’s Youtube channel.
Vitamin B3 (Nicotinic acid– most important and not nicotinamide or other forms) – Vitamin B3 has been cited as a building block of NAD and NADP. NAD+ is released during the early stages of inflammation and has immunomodulatory properties, known to decrease the pro-inflammatory cytokines, IL-1β, IL-6, and TNF-α. Recent evidence indicates that targeting IL-6 could help control the inflammatory storm in patients with COVID-19. Groups I belong to say that 500mg is too much and that flushing can feel unpleasant, so it’s best to take smaller amounts with food to reduce the flushing effect. Please consult your doctor for more details on dosage or if it’s appropriate for you. I have been using this supplement for the past few weeks and am not certain of its benefits since I feel pretty much the same. However, I am 95% healed at this point, so it likely has a much greater benefit for those who are more severely ill or experiencing fatigue. I have heard as much from threads on reddit and Facebook. Taking 500 mg or more of nicotinic acid or nicotinamide may trigger autophagy, which is not recommended more than about once per week according to Tom Bunker of RecoverFromLongCovid.com.
Prescription Medications You Might Consider
Chronic Covid-19 has a litany of symptoms and not all of them can be effectively treated with OTC medications or supplements. Deregulation of mast cells can activate and release both inflammatory histamine and serotonin into the body. This serotonin boost can induce anxiety in the host. If you are experiencing increased levels of anxiety, you may talk to your doctor about a prescription that can relieve these symptoms. Mast cell activation can also lead to skin rashes and other allergic reactions that may occur. Before accepting a prescription for a new anti-anxiety or anti-depression medication, please do your homework and learn about all of the potential risks, side effects, and safe dosages that will not lead to addiction. Many of these drugs can become extremely addicting and require a tapered dose approach before quitting to avoid severe and sometimes fatal withdrawal symptoms.
Take this section with a grain of salt, since so much of the data is emerging. Some is very promising, but we’ve seen those hopes dashed before. If any of the treatments below are debunked, I will remove them and add a note. These are prescriptions that some survivors believe have helped them in various phases of the disease. They also have a good deal of support from the medical community, but also some pushback due to lack of evidence that could take months or years to indisputably prove.
Fluvoxamine – There is a lot of buzz around this antidepressant drug for it’s anti-inflammatory properties that appears to be effective at keeping Covid patients out of the hospital. This has been long talked about in the long hauler community as an effective treatment for brain fog.
Methylprednisolone – This steroid has apparently “cured” some long haulers as documented by Dr. Been. Dr. Been claims he has cured 100% of his long hauler patients with either one 5-day round of oral methylprednisolone. There was one minor exception, which he explains in the video. You may ask, “Why haven’t you taken methylprednisolone yet?” The answer is that I have only recently found out about this and I am scheduled to have an endoscopy to make sure I don’t have a bacterial overgrowth, which my GI doctor suspects and are not uncommon following rounds of antibiotics, steroids, or acute infections. Since steroids can lead to bacterial overgrowth, I don’t want to exacerbate the issue before the procedure. Once cleared and I rule out that whatever is going on in my gut is not the reason for my ongoing symptoms, I will ask my doctor for a course of methylprednisolone.
Ivermectin – Ivermectin has become the butt of a lot of jokes since the media ran with the story of it being a horse drug. While it is widely used on livestock and horses to fight parasites, it’s also a human drug that won the 2015 Noble Prize for curing awful human diseases like River Blindness and Lymphatic Filariasis. It is widely available around the world and sold in the United States as Stromectol (oral) and Soolantra (topical cream) and Sklice (topical cream). While Ivermectin is routinely prescribed for pets, including horses, so is aspirin and many other drugs that humans are given. Ivermectin has been given to humans over 3.7 billion times and is considered extremely safe. Some physicians are using it for active Covid and others are using it to treat long haulers. The NIH just updated their guidance on Ivermectin allowing healthcare providers the option of using it, even though the NIH neither recommends for or against using it at this point. I have taken two doses of 12mg each on Day 0 and Day 4 of Stromectol (Ivermectin). Two weeks after treatment with both Ivermectin and Maraviroc, my GI symptoms cleared and have not returned. Ivermectin has also been shown to promote peripheral nerve regeneration in this 2018 NIH paper.
Maraviroc – This is an antiviral drug created to treat HIV infection. Dr. Patterson prescribed this for me, but I am still awaiting pharmacy approval. I was prescribed a one week course of this medication to take twice a day. My results are discussed in the section above.
Leronlimab – This monoclonal antibody was developed by Cytodyn Inc. and targets the CCR5 receptor found on T lymphocytes in the immune system. Originally, it was developed for the treatment of HIV and breast cancer but was granted emergency use authorization for the treatment of mild to moderate Covid-19. Cytodyn are conducting trials of this drug for long haulers, but results are still pending in the clinical trial data found here.
Bamlanivimab – This is another monoclonal antibody developed by Eli Lilly for the treatment of Covid-19. So far I have only heard of this drug being used for use in hospitalized patients. I will update once I hear about any uses for Chronic Covid.
Autonomic Dysfunction and Bizarre Symptoms
As I mentioned above, the best way I can describe my Covid-19 experience based upon past traumas would be a severe concussion. I’ve had concussions before and what Covid-19 did to my brain, nervous system, and body was far worse than anything actual head trauma I’ve experienced.
If you are a long-hauler and experiencing any crazy symptoms that involve blood pressure and heart rate changes, please watch this webinar with Dr. Svetlana Blitshteyn of the Dysautonomia Clinic.
Brain Fog and the Glymphatic System
The Glymphatic System is also known as the brain’s sewage system. It wasn’t discovered until 2012 and serves as your brain’s version of the body’s lymphatic system. Essentially, it clears out waste from the cerebral spinal fluid in your brain. A good night’s sleep and keeping inflammation down are keys to keeping this system working efficiently. When inflammation occurs, this system can get backed up and lead to brain fog or pressure.
Here are some exercises you can do to help move out the fluid and relieve your symptoms. I’ve also been told that moving your neck and spine can help relieve pressure as well.
The Vagus Nerve and the Brain/Gut Connection
The vagus nerve is the longest cranial nerve in the body that winds its way from the brain stem all the way to part of the colon. If you’ve experienced autonomic dysfunction as I have you might feel something happening in your gut in your head moments before you feel it in your gut. It generally feels like a small wave of anxiety right before your gut gurgles.
The vagus nerve is a key component of your parasympathetic nervous system which keeps your fight-or-flight mechanism in-check. So when your parasympathetic nervous system is out of whack, you may experience all sorts of uncomfortable symptoms, including:
- panic attacks
- unusual heart rate
- difficulty speaking or hoarse voice
- ear pain
- trouble drinking
- abnormal blood pressure
- nausea and vomiting
- abdominal pain or bloating
- changes in blood sugar
- weight loss
- acid reflux
- and more!
There are simple ways of stimulating this giant, wandering nerve to get your body back on track, including gargling, cold water in the face, cold shower, and some exercises found in the video below.
Physical exercises to stimulate the Vagus Nerve system.
Breathing exercises to stimulate the Vagus Nerve and calm the nervous system.
Massages that stimulate the Vagus Nerve.
Should a Long-Hauler Take The Vaccine?
Should a long-hauler risk taking the vaccine when it is available to them? A study of 473 long haulers who have taken the vaccine may help you make up your mind.
There was also a poll on Reddit that asked Long-Haulers who took the vaccine how they fared. The comments can be read here.
Prophylaxis & Early Outpatient Treatment
I-MASK+ Protocol
The new I-MASK+ protocol was authored by Dr. Paul Marik who also published the MATH+ protocol for in-patient care. I-MASK+ focuses on preventive or prophylaxis and early outpatient care. It encourages use of Ivermectin (anti-parasitic drug) that has a strong safety profile since its introduction in 1987. Hospitals around the world have been recording great success with its use in every phase of the disease. The video below talks about this in detail and the protocol can be found here.
Mouthwash Fights Covid?
It sounds too good to be true, but there is evidence that supports that using antiseptic or povidone iodine-based mouthwash and/or nasal rinses can prevent coronaviruses from replicating in the upper respiratory tract. This does not mean that antiseptic mouthwash, like Listerine Cool Mint, kills the coronavirus that causes the Covid-19 disease, but recent studies support that using it 3 times per day for at least 30 seconds can reduce the viral load detected in people exposed to the virus.
Listerine Antiseptic Cool Mint is named specifically in at least one of the studies which are considered anecdotal evidence at this point. Listerine’s statement casts doubt on the effectiveness of their product against disease-causing viruses as you might expect.
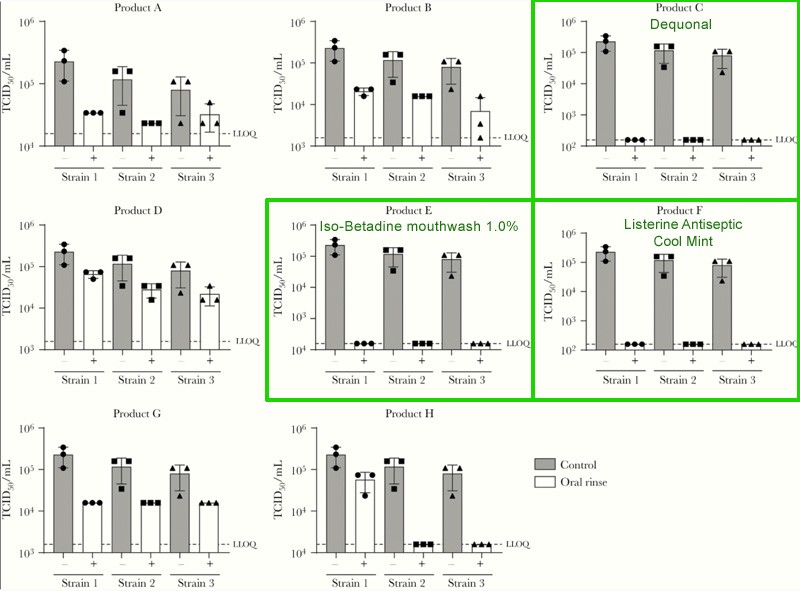
Study published in Oxford Academic under the The Journal of Infectious Diseases, Volume 222, Issue 8, 15 October 2020, Pages 1289–1292.
Yahoo Article discussing deactivation of virus.
Study using povidone iodine in Malaysia.
Social Media Support Groups
I have one big caveat with these groups. While they have been instrumental to my validation and understanding of this disease, they can be a double-edged sword sometimes. Most people post on these groups to tell you about their worst day or vent about lack of care and that can be extremely distressing to a reader. There are attempts by many to post positive messages as well more recently, so just keep that in mind and know that negative posts are the driving force of social media in general. It’s a huge part of the reason we are living in such a divisive time right now. Definitely monitor your time on these groups and take note of how you felt before and after reading. Reducing stress is a key part of recovery, so take a break when your body is telling you that you need one.
| Survivor Corp – Facebook |
| Covid-19 Longhauler Advocacy Project – Facebook |
| Long Haul COVID Fighters – Facebook |
| Long Covid Support Group – Facebook |
| Covid Long Haulers – Reddit |
| Body Politic – Slack |
| Ivermectin MD Team – Facebook |
YouTubers I Follow for Covid-19 Medical Information
My Story
In early March 2020, I was dealing with terrible headaches and toothaches without any perceptible dental cause. My PCP sent me to the dentist who sent me to the ENT who then sent me back to the dentist. The pain was so excruciating every time I breathed, I taped off my right nostril to prevent any airflow into my right sinus cavity. Little did I know that was just the beginning of what would be the most frustrating and life-threatening health rollercoaster ride of my life.
On March 13th, I was diagnosed with “acute viral sinusitis” and given Amoxicillin to relieve whatever was going on in my sinuses. By the morning of March 16th, the pain had subsided and I thought I was in the clear. I could finally breathe normally again without any pain! But as I was preparing to go to sleep that night I began experiencing sudden shortness of breath. It didn’t make any sense to me as my airways felt clear. I grew up with Asthma so I knew this was something entirely different.
When I laid down, my pulse shot up rapidly and it felt like my head was going to explode from enormous pressure building. I sat back up and simply focused on trying to breathe but I never felt like I was in control of my diaphragm. It was as if my body suddenly forgot how to breathe. I stayed up that entire night and by morning started experiencing rolling arrhythmias that left me dizzy and feeling like I would blackout. This felt like nothing I’ve ever had in my life. Not H1N1 that I caught in Japan in 2009, asthma attacks or any of my many bouts with bronchitis ever came close to how intense this was. This felt completely alien to me. In hindsight, I believe the sinus arrhythmias were caused by my rapid and uncontrollable breathing pattern.
I talked to a friend who convinced me that I was having a serious cardiac event, so I drove to the Emergency Department at my local hospital. After waiting several hours they brought me in and ran X-rays of my chest, gave me an EKG, took blood, and then sent me home. Since I didn’t display the telltale signs of known Covid-19 at the time, they assumed it was just anxiety, panic attacks, sinus arrhythmia, and “acute viral sinusitis.” I was not tested for Covid-19 since testing was not widely available in Oregon at the time and was reserved for those admitted to the hospital. Even though I had no history of anxiety or panic disorder, I don’t blame the staff since it would be many weeks later until Covid-19 was recognized as an endothelial disease that can cause autonomic dysfunction. It was also not widely known that loss of taste and smell were symptoms, which I also experienced.
I spent the next two nights sitting up and just focusing on breathing. My lungs didn’t seem to want to open after I exhaled. Every time I began to nod off, I would suddenly stop inhaling. I watched dozens of YouTube videos on breathing techniques and no matter what I did, I could not control the rhythm of my breathing. When I tried to lay down flat, my heart would feel like it was about to explode out of my chest, but would eventually settle down when I sat back up. I did not understand what could be causing this. I had never heard of dysautonomia or POTS before. While I had known several people with extreme anxiety and panic disorder and I never witnessed them going through a panic attack lasting days without ever letting up. Since I read that you can’t die from a panic attack, I allowed myself to pass out while sitting upright and just thinking to myself, “If I die, I die.” It was the first time I slept in three days, but it didn’t last long. At one point in the night, my body slumped out of the upright sitting position and awoke in a panic attack. I spent the next several months trying to sleep upright with limited success.
I continued treating my symptoms as if they were related to anxiety for months, but could not understand why I had this intolerance to laying down out of nowhere. Was it PTSD? I didn’t feel any anxiety before laying down. My heart would just start racing the moment it felt horizontal. It completely baffled me and my PCP. I felt spaced out and dizzy when I would stand up and walk around and at times felt like I was controlling myself outside of my body, similar to a third-person video game. I took three separate anxiety tests and registered as not showing any signs of anxiety or depression. I spoke to a psychiatrist who told me he didn’t see any reason for us to continue having conversations as he didn’t believe I had anxiety.
The other big issue that I couldn’t understand was why I kept having weekly relapses that landed me in bed for days at a time. These flares left me feeling completely sick and exhausted. I would have freezing cold extremities and feel like my core was burning up even though my thermometer readings were normal. It seemed to be related to inflammation, so I started on a very strict low inflammation diet. It seemed to help at least a little bit, which was reason enough to continue it. I read that intermittent fasting could help accelerate the body’s healing process, so I started adopting that as well. From March until September I would lose 40 pounds on this diet.
It wasn’t until July 2020 until I found Dr. Noah Greenspan on a Facebook Long-Haulers group and my whole perspective changed. I told him my story and he said it was exactly the type of Covid-19 cases they were seeing in NYC since the beginning of the outbreak. The Dysautonomia and POTS clinics went from seeing one new patient a week to seven since the start of the pandemic. Finally, I had answers that made sense. I didn’t want to accept that I had somehow contracted a brand new unknown disease, but at least it was a place to start.
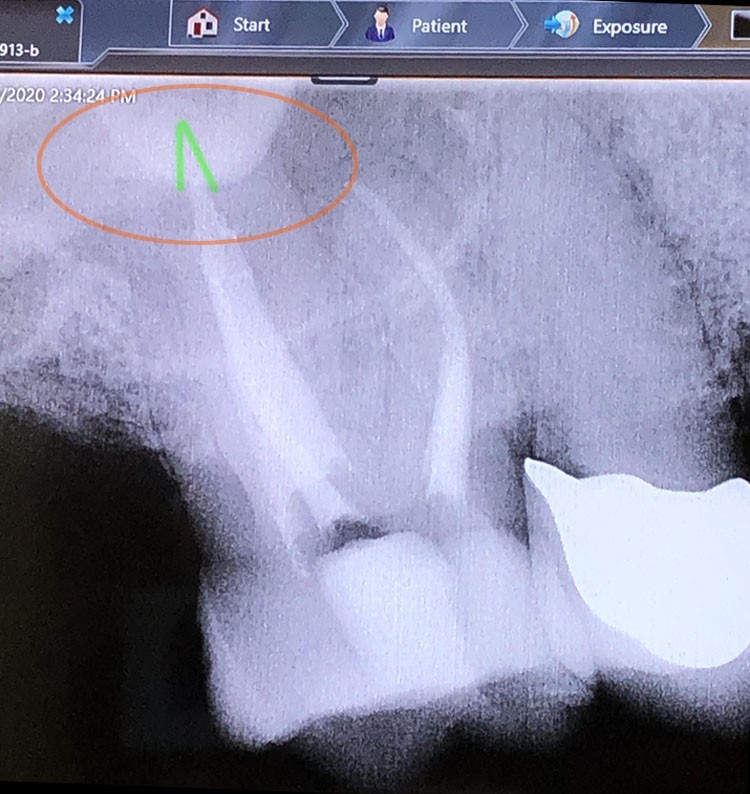
I had left out what was occurring in my sinus cavity since I thought it was unrelated, but since I’ve been hearing more and more about dental issues I’ve decided to add this. In late February I was having acute pain in my upper right jaw. I’ve had abscess teeth before and this felt more severe than that pain. It radiated around my jaw and right side of my head resulting in terrible headaches. The dentist looked around, took X-rays and told me that everything looked fine. I then visited a ENT who performed a CT scan and discovered that the sinus end of a back tooth had decayed and exposed a nerve within my sinus cavity. The tooth was otherwise healthy! The antibiotics I took seemed to take care of the pain and allow me to breathe out of the right nostril again, but then came all of the most serious symptoms mentioned above. I didn’t get a root canal until another month after my ER visit.
Change Log
- Update: 10/28/2021 – Brief paragraph on neuroplasticity (2 paragraphs down) and updated charts
- Update: 6/14/2021 – Updated new video of Dr. Svetlana Blitshteyn regarding Dysautonomia under the Keys to Recovery section
- Update: 5/13/2021 – Update on my Pfizer vaccine dose reactions. Updated sections on Ivermectin, Maraviroc, and Sleep.
- Update: 3/3/2021 – Updated section about Anxiety and how adrenaline is released to combat histamine. Added new section about Vaccines.
- Update: 2/9/2021 – Latest update on IncellDx’s medications. New video regarding Mast Cell Activation Syndrome and Long Covid.
- Update: 1/26/2021 – More updates on my results and medications from IncellDX’s long hauler program.
- Update: 1/16/2021 – (NIH update on Ivermectin and my results from IncellDX’s new long hauler program)
- Update 1/15/2021.1 – Added links to IncellDX and Dr.Yogendra’s new Long Hauler program.
- Update 1/15/2021 – Updated Gut section and added great Long Hauler video from PBS NewsHour. Added my dental account to My Story.
- Update 1/14/2021 – Updated section regarding Gut Health and my endoscopy results. Added several links to articles regarding gut health and Covid.
- Update 1/10/2021 – Updated prescription medication section with Leronlimab, Maraviroc, and Bamlanivimab. Added new annotated symptom chart image.
- Update 1/8/2021 – Update on flare-up after drinking whiskey.
- Update 1/7/2021 – Updated RUN-DMC’s supplement video with a newer one. Updated section on alcohol.
- Update 1/4/2021 – Added Medcram video on IVM. Edited My Story. Added section regarding MCAS and Alcohol. Updated & fixed link to Google Sheet and Excel file.
- Update 12/24/2020 – Added more to intro. Added section on fasting. Added Anxiety symptom and cause. Added videos by RUN-DMC and Dr. Yo.
- Update 12/17/2020 – Revised intro. Added video interview with Dr. Bruce Patterson.
- Update 12/9/2020 – Added new RUN-DMC video interview with Nikita Alexandrov regarding NAD+ and added Dr. Been video regarding IVM.
- Update 12/1/2020 – Updated Supplements with Black Cumin. Added Secondary Infections section. Added Ivermectin MD Team group. Edited Story.
- Update 11/17/2020 – Added to Vitamin B3 section and removed Niacin. Added new primer video by Run-DMC. Added new supplements.
- Update 11/16/2020 – Added new Vitamin B3 paragraph. Added new video regarding Ivermectin. Added advice about normal daily aches and pains.
- Update 11/14/2020.2 – Added comment regarding Ivermectin’s ability to heal peripheral nerves.
- Update 11/14/2020.1 – Added section called What Does Chronic Covid-19 Feel Like?
- Update 11/14/2020 – Added mention of CDC’s official recognition of the condition. Added The 5 Month Mark section. Expanded on Vitamin D3 section.
- Update 11/12/2020.1 – Added Ivermectin under prescription medications.
- Update 11/12/2020 – Added video regarding the potential of viral persistence. Added section on social media support groups.
- Update: 11/11/2020 – Added sections regarding Prescription Drugs and Prophylaxis including the new I-MASK+ protocol
- Original Post Date – 10/13/2020
- Update: 11/4/2021 – Radio interview with local NPR
Notations
1 Credit to reddit user penguina83 for describing it as “like hanging upside-down for hours”

